Lower Back Pain and Sciatica
- Mar 2, 2018
- 12 min read
Almost everyone will experience lower back pain at least once in their lifetime, with an estimated 5%-10% of patients with low back pain having sciatica, whereas the reported lifetime prevalence of low back pain ranges from 49% to 70%. The annual prevalence of disc related sciatica in the general population is estimated at 2.2% ("Diagnosis and Treatment of Sciatica", Koes, B W, M W van Tulder, and WC Peul, 2018). These statistics highlight the importance of understanding the reason for lower back pain, and the concerning levels of how chronic the situation can get, particularly if not dealt with.
Most people consider NSAID's (Non-steroidal Anti-Inflammatory Drugs) a sufficient way to deal with the pain as they help relieve the symptoms. However, there is increasing awareness of the over use of pain killers on both the immune system and liver, and unless dealt with physically, it is more likely to return and thus, become chronic. Therefore, this displays the importance of dealing with lower back pain physically by correcting the issue directly, rather than "masking" the issue and hoping NSAIDs work. Here I aim to show ways in which you can do this, by explaining the various causes of lower back pain, and realistic and manageable ways to help relieve the pain properly. It must be noted that moderate use of NSAIDs is acceptable unless your doctor has advised otherwise, with the understanding that NSAIDs simply deal with the pain, and commonly not the cause. NOTE: If you are taking NSAIDs, it is important you DO NOT take any pre-treatment as it increases risk of worsening the situation.
COMMON CAUSES OF LOWER BACK PAIN:
1) Anteriorly (forward) rotated pelvis aka Lordosis
2) Sciatica
3) Breathing Dysfunctions
Questions I ask my clients:
- How curved is your lower back?
- Do you stand and lie down with hyperextended knees?
- When you lie down on your back, how far off the ground is your lumbar spine? And is one SI Joint off the surface more than the other, ie. is there more pressure on one of your glutes?
- In standing, how much pressure do you put down your heels?
- How much pressure do you put down your big toe compared to the outside of your foot? Does the pressure differ between each big toe and foot?
- Are the arches in your feet high, average or collapsed/fallen?
- Can you feel one hip bone on the front (ASIS) more than the other?
- Is more weight down the front of your leg or back of the leg (ie. Quads or Hamstrings)?
- Do you breathe into your gut, chest or shoulders?
A fun exercise to show how the pelvis balances (requires more than one person):
Stand facing each other, and taking it in turns, the first person gently pushes the others shoulders backwards as they stand with feet rotated outwards (laterally rotated). DO NOT push too hard as this is the weaker position, be respectful and appreciate what it is showing. Then the person rotates their feet inwards, and repeat gently pushing the shoulders back.
With the feet laterally rotated, the hip stabilisers are not acting sufficiently as the pressure is being absorbed more by the lateral rotators, therefore, I describe this as the stilletoe heel in sand as the spine receives more pressure. With the feet rotated inward, the hip stabilisers are in a stronger position, allowing for absorption into the whole pelvis, meaning less pressure into the spine, and thus, I describe this as the elephants foot in sand.
1) ANTERIORLY ROTATED PELVIS aka LORDOSIS
In simple terms, the support of the arch in your foot comes from the hip stabilisers which are glute min and mede.
The balance of the pelvis depends on how the feet and knees absorb the pressure, and also superiorly in regards to the balance of the torso. In some cases, the shoulders, head and jaw can be imbalanced due to the lack of support from the feet/a foot which compensates through the leg and hip!
Moving upwards:
Laterally rotated feet means less support for the tibia, placing increased pressure on the outside of the foot and less use of the big toe (noting the big toe, physiologically known as the hallux, is vital for balance), which can create fallen and collapsed arches. This creates imbalanced pressures into the knee, causing it to collapse inward as a result of the lack of tibia support which is physiologically known as a knee valgus. Knee valgus creates strain on the hip as the glute min and mede switch off, meaning increased strained tension in TFL and IT Band, and more pressure on the groin and hip flexor insertion at the top of the medial (inner) femur.
In terms of performance, laterally rotated feet cause the tibia and fibia to twist outwards meaning the outer half of the calf (gastrocnemius and soleus muscles) are worked more, and with the lack of use of the big toe creates more pressure on the plantar plate. Moving upwards, as the tibia and fibia twist outwards, the femur twists outwards and collapses inwards to compensate, meaning the more pressure on the MCL and twisted strain on the LCL, and causing the ACL and PCL to twist and absorb imbalanced pressures in the knee joint. As the femur rotates and collapse, the quads become more like the IT Band, IT Band more like hamstrings, hamstrings more like adductors, and adductors like quads, noting the iliopsoas (hip flexors) insertion is now absorbing more pressure as the balance is placed on the groin. With the tension into the iliopsoas increases, it pulls on the lower back, and consequently tilting the pelvis forward, ie. anteriorly rotated pelvis.
Moving downwards:
From Kyphosis - The more kyphotic in posture, the more pressure created on the anterior chain (front of the body) in terms of balance against gravity. As stated in a previous blog (Stress in the Neck and Shoulders), Julian Baker at the British Fascia Symposium 2016, put forward that the SCM (a neck muscle) is a hip flexor, noting the back and forth movement of the neck in sprinters. In order for the body to maintain an upright posture with increased pressure on the anterior chain, tilting the body forward, the hip flexors are required to absorb the tension from the lower back to legs, via the pelvis. As the hip flexors become more hypertonic, they shorten causing the pelvis to anteriorly tilt!
From sway back posture - With the head behind the hips, it creates increased tension in the back extensors, shortening the gaps between spinal processes in the lumbar area (lower back), and SI Joints absorb abnormal pressures into the pelvis.
Ultimately, it can be recognised with weakened abdnominal muscles, tight back extensors, hip flexors and quads, causing weakness in the antagonistic glutes and hamstrings.
TOP TIP: If you think you are walking pigeon toed (toes in), you are likely to be walking with straight feet. It may feel odd to begin with, but the more you do it, the easier it will become. It is important to do this without looking down as looking down puts more pressure on the anterior chain. Ensure there is the straight line between ear, shoulder, hip, and ankle. Compare the pelvis to a bucket of water, tip too far forward or back and the water will spill.
TOP TIP: Towel scrunches with feet inwards and square pelvis. This will help mobilise the connective chain from big toe to hip in the correct way.
TOP TIP: Glute bridges with feet and knees straight and in line with the hips, and hips in line with the shoulders. Make sure the big toe is engaged throughout, and that you are using the whole pelvus. Gently roll each vertebrae of the ground using the glutes to power the movement, and then gently roll each vertebrae back down, ensuring chain between big toe and hip is balanced and engaged throughout. Note, the knees may try and collapse in or out due to tension, try and maintain straightness, even if it means you cannot move up too far, as it will increase with practice.
TOP TIP: Uphill walking ensuring toes are facing in, using the big toe (curling and pushing down), knees are straight, pelvis is square, shoulders back and down and head retracted. The concept of keeping the bucket of water full analogy is very helpful here, as it puts more pressure on the glutes, including hip stabilisers (ensuring feet are straight and using big toe). This then engages the hamstrings more, and allows the quads and hip flexors to focus more on moving uphill, and less on posture. This links in with slow and fast twitch muscle groupings.
2) SCIATICA
Repeating what was mentioned above, an estimated 5%-10% of patients with low back pain have sciatica, whereas the reported lifetime prevalence of low back pain ranges from 49% to 70%. The annual prevalence of disc related sciatica in the general population is estimated at 2.2%("Diagnosis and Treatment of Sciatica", Koes, B W, M W van Tulder, and WC Peul, 2018). It is evident that many people suffer with sciatica at some point, and the location of pain can vary depending on the cause. In some cases, as above, it can be due to a herniated disc, which is where the spinal disc moves forwards and/or sideways and presses on the sciatic nerve. In this case, a course of physiotherapy, sports massage, and chiropractic or osteopathy treatment is recommended, noting it is important to not take any NSAIDs before treatment to avoid risk of further injury.
If the sciatica is not due to a herniated disc, it is usually due to the piriformis muscle. The sciatic nerve leaves the spinal cord between spinal processes L5 and S1 which is where the lower back meets the pelvis, and travels down through the pelvic cavity to the leg, and down to the foot. In the pelvic cavity, it passes just anterior to the piriformis muscle which is a prime lateral rotator for the hip/leg, meaning the more the hip/leg is laterally rotated, the shorter this muscle becomes. Therefore, the more hypertonic the piriformis becomes, the more likely it will compress the sciatic nerve. This pain can be localised to the glutes, or it can travel down the leg as far as the foot.
TOP TIP: "Running Man" exercises, this is a complicated exercise to explain in writing, so I recommend watching this video from Tim Hill of "You Tonic" (SRMT, Nutritionist PT) who made me aware of this exercise - https://www.dropbox.com/s/i9w3zp9plewdfxz/Running%20Man.mp4?dl=0
TOP TIP: side steps using a resistance band around the knees and/or ankles, focusing on keeping both feet facing slightly inward, and standing upright keeping the "bucket full", shoulders back and down, and head retracted.
TOP TIP: Abduction in standing or sideline, ensuring toes are slightly inward and knees do not collapse in or out, and the pelvis and leg does not rotate.
TOP TIP: Lateral rotator, hamstring (ensuring square pelvis), and adductor stretches. Quad and hip flexor stretches are also helpful. "Banana Stretches" are also good if there is more than one of you. Note- Try keeping the big toe a little curled (initiating an arch in the foot), and facing slightly inward for hamstring stretches, and pushing down into the surface with the big toe on the adductor stretches. For quads and hip flexors, it is a hip flexor stretch if you can see your knee, and if not, it is predominantly a quad stretch, and again noting that the pelvis is square.
3) BREATHING DYSFUNCTIONS
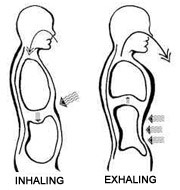
We have 12 pairs of ribs, with the lower 5 ribs being "false" and "floating" ribs giving them a greater capacity potential, compared to the 7 pairs of ribs attached to both the spine and sternum. Furthermore, our lungs are smaller at the top, and larger at the bottom with increased circulation supply to the lower parts, and our primary breathing muscle is the diaphragm. A functional respiratory diaphragm should move down on the inward breathe which pushes the gut outwards, and back up on the outward breathe, pulling the gut back in! During such inhalation and exhalation, it also mobilises the heart through attachments to the pericardial bag, the kidneys move up and down the central tendon, the stomach and pancreas down and left, the liver down and right, and the intestines move completely! Thus allowing for increased mobility of the gut, and thus, a more functional gut with the healthy elasticity and tensegrity relationships!
Only on exertion should we use the accessory breathing muscles, which recruits more chest breathing. Such accessory muscles include the scalenes, pectoralis minor, serratus anterior and both pairs of serratus posterior muscles.
In regards to easing lower back pain, when not using the respiratory diaphragm sufficiently, there is less movement into the abdominal cavity. There is also piezoelectricity potential into the abdominal and pelvic cavities as the respiratory diaphragm moves and compresses on the GI Tract, of which is lacking in dysfunctional breathing patterns. Abdominal breathing allows movement into the mesentery (recently discovered as an entire connected organ rather segmented: The mesentery: structure, function, and role in diseaseCoffey, J Calvin et al.The Lancet Gastroenterology & Hepatology , Volume 1 , Issue 3 , 238 - 247). Furthermore, it allows movement into the greater and lesser omentum and subcantaneous tissue of the gut, which is a common store of visceral fat. Overall, it increases the likelihood of tension at the diaphragm attatchment at the spine at T12-L2, which impacts the psoas muscles (the main hip flexors) which has attachments to all aspects of the anterior lumbar transverse processes, and the antermedial aspect of all lumbar discs and adjoining bodies (excluding the disc between L5 and S1). Therefore, reduced respiratory diaphragm movement means less recoil into the gut, causing increased potentials of gut tension, including organs, such as the kidneys no longer move up and down the central tendon. And physiologically, there is a greater chance of postural deviants, such as an anteriorly rotated pelvis due to the tension transferrred into the psoas, kyphosis due to the assisted breathing muscles becoming more primary in the movement, storing tension in the neck and shoulders. As the areas become more tight and strained, it can pull on the aponeurosis of the lumbar (a white tendinous sheeth inserting into the iliac spine), which can pull and strain the SI Joints, and thus creating imbalance and painful symptoms.
I also advise this with clients who suffer from IBS, as abdominal breathing can help relieve the twisting gut feelings, reducing gut tension and allowing more function into the GI Tract.
Dysfunctional breathing patterns:
1. Hyperventilatory: Rapid-breath pattern (averaging 20 breaths/minute) uses accessory muscles and restricts diaphragmatic movement being predominantly (thoracic patterns) in nature. Sometimes produced from poorly managed anxiety, this pattern manifests as very shallow, very rapid, and compounded by sputtered sighs (periodic patterns) and gasps (clavicular patterns). Panic, anxiety, and shock habituate this common phenomenon. People exhibiting this pattern immediately imperil their health.
2. Thoracic: These “chest-breathers” lack significant abdominal movement, with shallow and costal breaths. Enlarging thoracic cavity creates a partial vacuum by lifting the rib cage up and out through external intercostals muscles. Although the lungs do manage to be expanded by negative pressure, it is not enough to ventilate the lower lobes. This reduces pulmonary ventilation, since the lower lobes receive the greatest blood volume due to gravity.
3. Periodic: This pattern demonstrates rapid-shallow breathing, followed by a holding of breath, followed by a heavy sigh due to excessive CO2 concentrations in the bloodstream. This pattern flushes the CO from the bloodstream, which causes the brain’s autonomic system to shutdown respiration until the CO2 level raises to appropriate gas mixture. In the Periodic pattern, this cycle perpetuates. This is not to be confused with true apnea, and can be diagnosed by witnessing that the pattern does not cause a change in color, such as no blueness of the lips, and the individual resumes shallow, rapid breathing without intervention, following the sigh. This pattern can be created through sustained anxiety, or by post-traumatic stress syndrome.
4. Clavicular: This pattern exhibits chest-raising that elevates the collarbones while drawing in the abdomen and raising up the diaphragm. People who are “open-mouth breathers” attempt to increase intake through oral inhalation, but this provides minimal pulmonary ventilation. Worse still, the accessory muscles used in this pattern consume more oxygen than it provides. In exercise, these individuals fatigue quickly.
5. Paradoxical: Often called “reverse” breathing, this abdominal pattern contracts during inhalation and expands on exhalation (using the muscles for the opposite purpose for which they were intended, thus, paradoxical/reverse.) Paradoxical breathing associates with the expectation of exertion, sustained effort, resistance to flow, and stress. Through stress, shock and fear, people can condition themselves to inhale (often married to clavicular and thoracic patterns), followed by hypoxic breath-retention and periodic sighs. As a result, this pattern causes very rapid fatigue.
6. Hypoxic: In preparation
of perceived exertion, this pattern comprises an inhalation, withholding of exhalation (breath retention) until the perceived exertion concludes. Holding the breath dramatically increases intra-thoracic pressure, causing health risks such as, fainting associated with vagal nerve stimulation, increase in blood pressure, and hypoxia (reduced oxygen levels). Chronic baseline hypoxic breathing is very common, especially in "athletes”, due to conditioned exertion. Hypoxic patterning connects with the "flight-fright-freeze" response, predominantly more "freeze", the defense mechanism of “bracing” caused by anxiety.
TOP TIP: If you find it difficult to activate the respiratory diaphragm in abdominal breathing, try lying down as reducing the pressures of gravity in this way can help it's mobility. Also, speak to a Physical Therapist, ensuring they are aware of dysfunctional breathing patterns and how to correct them. Soft tissue treatment on the abdominals is very helpful, ensuring the movements aid the direction of the GI Tract, and therefore, I strongly advise speaking to a medical professional such as physical therapist or GP before doing so. For therapists, techniques that can be help include the Douglas Heels Technique, Muscle Energy Techniques to increase recoil, Soft Tissue work including Myofascial Release of which MFR of the belly button is particularly helpful, Frequency Specific Micro-Currents (FSMC), and Feldenkrais.
References:
- Koes, B W, M W van Tulder, and W C Peul. “Diagnosis and Treatment of Sciatica.” BMJ : British Medical Journal 334.7607 (2007): 1313–1317. PMC. Web. 1 Mar. 2018.
- https://www.fxmedicine.com.au/content/paracetamol-depletes-glutathione
- Bessone, Fernando. “Non-Steroidal Anti-Inflammatory Drugs: What Is the Actual Risk of Liver Damage?” World Journal of Gastroenterology : WJG 16.45 (2010): 5651–5661. PMC. Web. 1 Mar. 2018.
- Bancos, Simona et al. “Ibuprofen and Other Widely Used Non-Steroidal Anti-Inflammatory Drugs Inhibit Antibody Production in Human Cells.” Cellular immunology 258.1 (2009): 18–28. PMC. Web. 1 Mar. 2018.
- The mesentery: structure, function, and role in diseaseCoffey, J Calvin et al.The Lancet Gastroenterology & Hepatology , Volume 1 , Issue 3 , 238 - 247
- Anatomy and biomechanics of psoas major.Bogduk N, Pearcy M, Hadfield GClin Biomech (Bristol, Avon). 1992 May; 7(2):109-1
- Sajko, S., & Stuber, K. (2009). Psoas Major: a case report and review of its anatomy, biomechanics, and clinical implications. The Journal of the Canadian Chiropractic Association, 53(4), 311–318.

If you have any questions, please contact Kim and she will reply as soon as possible.
























































Comments